- Loading...
Fetal heart monitoring during labor provides a window into your baby's well-being. When doctors, nurses, or midwives fail to properly interpret warning signs on the fetal monitor strip, the consequences can be devastating, resulting in brain damage, cerebral palsy, or even death.
At the Jacob D. Fuchsberg Law Firm, our New York birth injury attorneys have decades of experience holding medical providers accountable when they ignore or misinterpret signs of fetal distress. We understand the medical science behind these cases and fight relentlessly to secure the resources your family needs.
Fetal Monitoring and Why It Matters During Labor
Fetal heart monitoring is a standard procedure used during labor to track your baby's heart rate and your contractions. This monitoring serves a fundamental purpose: detecting when your baby isn't getting enough oxygen.
Despite what some defense attorneys and hospitals claim, fetal heart monitoring is not just a formality. According to data from the American College of Obstetricians and Gynecologists (ACOG), fetal monitoring is used in nearly 85% of births nationwide because proper interpretation can warn the obstetrical team of potential complications that may lead to neonatal brain injury.
Common Types of Fetal Heart Rate Patterns
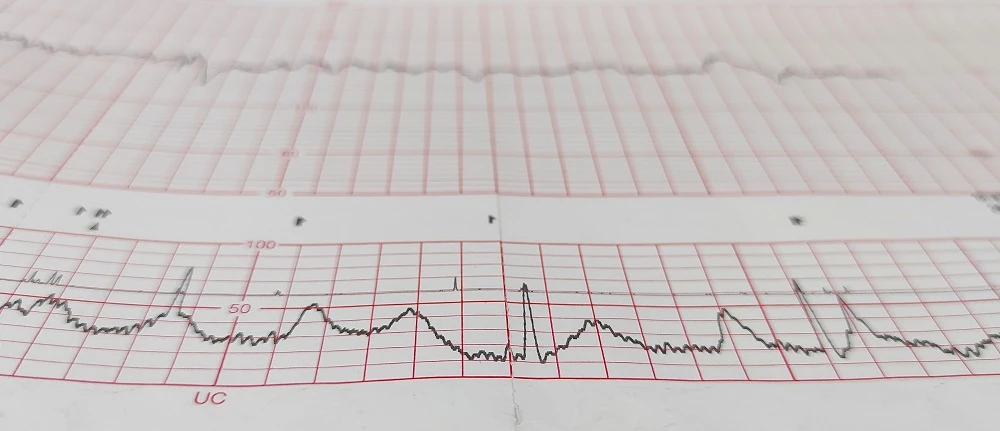
Medical professionals should recognize and respond to specific patterns that appear on fetal monitoring strips:
- Baseline heart rate: A normal fetal heart rate ranges from 110 to 160 beats per minute. Rates consistently above or below this range may indicate problems.
- Early decelerations: A gradual decrease in heart rate that coincides with contractions and returns to baseline is generally benign and may result from head compression during contractions.
- Late decelerations: Heart rate gradually decreases after a contraction starts, with the lowest point occurring after the contraction peaks. Late decelerations may indicate the placenta isn't providing enough oxygen to your baby.
- Variable decelerations: Abrupt drops in heart rate often result from umbilical cord compression and require immediate attention when severe or repetitive.
- Tachycardia: A baseline heart rate consistently above 160 beats per minute may indicate infection, maternal fever, or fetal distress.
- Bradycardia: A baseline heart rate consistently below 110 beats per minute can signal serious oxygen deprivation.
- Minimal or absent variability: Normal babies show some variability in their heart rate, and the absence of this variability often indicates distress.
How ACOG Guidelines Protect Doctors Instead of Babies
In 2009, the American College of Obstetricians and Gynecologists (ACOG) issued Practice Bulletin Number 106, establishing a three-tier system for classifying fetal heart rate patterns. Many plaintiff attorneys and birth injury advocates believe these guidelines were crafted with medical-legal protection in mind rather than infant safety.
The guidelines use ambiguous terms like "Category II" (indeterminate) that cover a broad range of concerning patterns. Rather than recommending preparations for prompt delivery when fetal heart rate patterns suggest potential compromise, the new guidelines essentially tell clinicians to "watch and wait" until the situation becomes an emergency.
This approach favors medical providers at the expense of babies. By the time a pattern is classified as "Category III" (abnormal), requiring immediate delivery, the baby may have already suffered irreversible brain damage.
Common Defense Tactics: How Hospitals Try to Disprove Fetal Monitoring Claims
When you file a lawsuit, don't be surprised when defendant doctors claim that fetal heart monitoring isn't predictive of brain damage or cerebral palsy. This defense contradicts the very reason they use monitoring in the first place.
Our experienced attorneys know how to dismantle these arguments using authoritative medical evidence. We cite prominent organizations like the New York Health Foundation and partnerships that work to study and standardize fetal monitoring practices.
We also use respected medical texts and articles that provide scientific evidence that a significant fraction of cerebral palsy cases involve oxygen deprivation during labor and delivery.
Markers of Hypoxic-Ischemic Encephalopathy
To prove your case, we must demonstrate that medical negligence caused hypoxic-ischemic encephalopathy (HIE), which is brain damage from oxygen deprivation. Key markers include:
- Low Apgar scores: Scores of less than 5 at both 5 and 10 minutes after birth indicate severe distress.
- Umbilical cord blood gases: A pH level below 7.0 or a base deficit of 12 mmol/L or greater confirms severe oxygen deprivation and acidemia.
- Neuroimaging evidence: Brain MRI or MRS scans may show injury patterns consistent with oxygen deprivation.
- Multi-organ failure: Damage to the kidneys, liver, heart, or other organs may be consistent with severe oxygen deprivation.
These markers reflect a physiological process where your baby became severely compromised during labor. As oxygen levels drop, the baby's body tries to compensate by increasing heart rate and shunting oxygenated blood to vital organs, including the heart, brain, and adrenal glands. If the condition persists, brain cells begin to die, particularly in areas responsible for movement, cognition, and breathing.
Additional Risk Factors in Fetal Monitoring Cases
Monitoring errors are often compounded by other forms of negligence, such as:
- Excessive Pitocin use: Pitocin increases the frequency, duration, and intensity of contractions. Overstimulation (tachysystole) can reduce oxygen flow to the baby between contractions, causing distress.
- Prolonged labor: Extended labor exhausts the mother and baby's oxygen reserves, making proper monitoring even more essential.
- Meconium-stained amniotic fluid: The presence of meconium (the baby's first stool) in the amniotic fluid indicates the baby experienced stress and increases the risk of serious complications.
- Abnormal fetal presentation: Babies in breech or other abnormal positions may not tolerate labor as well as those in normal head-down positions.
- Placental problems: Placental abruption (separation of the placenta from the uterine wall) or placental insufficiency can severely compromise oxygen delivery to your baby.
What Compensation Can You Recover?

Birth injuries from fetal monitoring errors often result in lifetime disabilities requiring extensive medical care, therapy, and support. New York law allows you to seek compensation for:
- Medical expenses: All costs related to your child's treatment, including hospitalization, surgeries, medications, medical equipment, and future care needs.
- Rehabilitation and therapy: Physical therapy, occupational therapy, speech therapy, and other specialized treatments your child requires.
- Home and vehicle modifications: Changes needed to accommodate your child's disabilities, including wheelchair ramps, accessible bathrooms, and modified vehicles.
- Lost earning capacity: If your child's injuries prevent them from working in the future.
- Pain and suffering: Compensation for your child's physical pain and diminished quality of life.
- Parental claims: Recovery for parental emotional distress, particularly when the child was stillborn due to medical negligence.
For qualifying cases involving birth-related neurological injuries, enrollment in the Medical Indemnity Fund provides lifetime coverage for medical care, rehabilitation, custodial care, durable medical equipment, home modifications, and more.
Steps to Take If You Suspect Fetal Monitoring Errors
If you believe fetal monitoring errors contributed to your child's birth injury, taking the right steps can protect your legal rights:
- Obtain all medical records: Request complete copies of your prenatal records, labor and delivery notes, fetal monitoring strips, and your baby's newborn records.
- Document your child's condition: Take photos and videos and keep detailed records of your child's diagnoses, treatments, therapies, medications, and how their injuries affect daily life.
- Preserve evidence: Save any correspondence with medical providers, bills, and insurance documents related to your delivery and your child's care.
- Don't sign releases: Hospitals and insurance companies may ask you to sign releases or settlement agreements shortly after your child's injury. Do not sign anything without consulting an attorney first.
- Contact an attorney quickly: Acting promptly preserves your rights and allows your attorney to gather evidence while it's still fresh.
Who Can Be Held Accountable for Fetal Monitoring Errors?
Multiple parties may share responsibility when fetal monitoring errors cause birth injuries:
- Obstetricians: Doctors who fail to properly interpret monitoring strips, delay necessary interventions, or make poor clinical decisions during labor.
- Labor and delivery nurses: Nurses who don't recognize concerning patterns, fail to notify physicians promptly, or inadequately document fetal status.
- Midwives: Certified nurse-midwives or other midwives who miss warning signs or fail to transfer care to a physician when complications arise.
- Hospitals: Medical facilities that have inadequate staffing levels, provide poor training, or have insufficient policies and protocols for responding to fetal distress.
- Anesthesiologists: Specialists whose medication administration causes or contributes to fetal distress without proper monitoring and intervention.
Our attorneys conduct thorough investigations to identify all potentially liable parties and pursue maximum compensation from each responsible party.
FAQ
Frequently Asked Questions
How do I know if fetal monitoring errors caused my child's birth injury?

Signs include concerning patterns on the fetal monitoring strips (late decelerations, bradycardia, absent variability) that were not acted upon, delays in performing a cesarean section despite non-reassuring patterns, and evidence of oxygen deprivation at birth (low Apgar scores, abnormal umbilical cord blood gases).
What is the statute of limitations for filing a birth injury lawsuit in New York?

Generally, medical malpractice cases must be filed within two and a half years of the alleged malpractice. However, for infants, the law allows claims to be filed until the child's 10th birthday in most cases, though earlier action is always recommended.
How long does a birth injury case take to resolve?

Birth injury cases involving fetal monitoring errors typically take two to four years to resolve, though this varies based on case complexity, the severity of injuries, and whether the case settles or goes to trial.
Can I afford to hire a birth injury lawyer?

Our firm handles birth injury cases on a contingency fee basis, meaning you pay no attorney fees unless we recover compensation for you. We advance all case costs, so there's no financial risk to pursuing your claim.
What if multiple medical providers were involved in my care?

We identify all potentially liable parties and pursue compensation from each one. This may include obstetricians, nurses, midwives, hospitals, and other healthcare providers who contributed to the negligent care.
Will I have to go to court?

Many birth injury cases settle before trial, but we prepare every case as if it will go to court. This preparation often results in better settlement offers, and if a trial becomes necessary, we're ready to fight for you.
Medical Negligence Shouldn't Rob Your Child of a Healthy Future
If your baby suffered brain damage due to fetal monitoring errors, our New York birth injury lawyers will investigate every detail of your labor and delivery records. We work with maternal-fetal medicine professionals to prove when medical staff failed to act on clear warning signs.
Your Baby Deserved Better Care
Fetal monitoring exists to protect babies during labor, and when medical staff ignore warning signs, they betray your trust. Our New York birth injury attorneys have recovered millions for families affected by preventable brain injuries and will fight to secure the compensation your child needs for lifelong care.

.svg)











